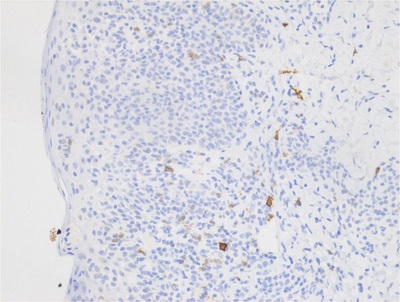
Immunostains:
Summary of IHCs: CD3+CD8+CD4-CD7-CD20-CD117-CD30-
Molecular test: clonal TCR gamma and beta gene rearrangement.
Diagnosis: Mycosis Fungoides, hypopigmented variant
Diagnosis: Mycosis Fungoides, hypopigmented variant
MYCOSIS FUNGOIDES
Definition: an epidermotropic, primary cutaneous T-cell lymphoma characterized by infiltration of small to medium-sized T-cells with cerebriform nuclei.
Epidemiology: MF is the most common type of CTCL, almost 50% of all primary cutaneous lymphomas. Common in adults/elderly, rare in children and adolescents.
M:F= 2:1
Sites: limited to the skin, with widespread distribution, for a protracted period. Extracutaneous dissemination may occur in advanced stages. Involving BM is rare
Clinical couse: patches to more infiltrated plaques and eventually tumours
Histopathology:
- classic epidermotropism
- Pautrier microabscesses (aggregates), or single cells
- cerebriform nuclei
- dermis infiltration: patchy, band-like, or diffuse
• Immunophenotype:
-CD2+, CD3+, CD5+, CD4+, CD8-, TCRb+
-CD7- (all stages)
- Cutaneous lymphocytic antigen (CLA) expressed in most cases
-Cytoxic granule associated proteins (-patch/plaque; +advanced lesion)
• Genetics:
- TCR genes clonally rearranged
- STAT3 activation, CDKN2A/p16INK4a & PTEN inactivation
- complex karyotypes, nonspecific
• Postulated normal counterpart:
- mature skin-homing CD4+ T-cell
• Prognosis and predictive factors
- clinical stage, >60 years, high LDH: poor prognosis
- large T-cell lymphoma transformation
Variants:
Hypopigmented variant
CD8+
Pediatric population, good prognosis
Pagetoid reticulosis
Patches or plaques with an intraepidermal proliferation of newplastic T-cell
•Infiltrates strictly in epidermis
- CD30+
- CD4+, CD8-; CD4-, CD8+
•Prognosis
- excellent
Folliculotropic MF
•Follicular infiltrates of atypical CD4+ T lymphocytes, often with sparing of the
epidermis
•Mucinous degeneration of the hair follicles
•Head and neck
Prognosis
- less favorable than “classical” mycosis fungoides
Granulomatous slack skin
•Slow development of folds of lax skin (axillae, groin)
•Granulomatous infiltrate with clonal CD4+ T cells, macrophages and multinucleated giant cells
•Indolent clinical course
Stage I
Disease confined to the skin with patches/papules/plaques, no LN involvement
Stage IA: <10% of the skin surface
Stage IB: >10% of the skin surface
Stage II
Stage IIA: with early (N1-N2) LN involvement
Stage IIB: One or more tumors are found on the skin (>1cm)
Stage III
Nearly all of the skin is reddened (erythroderma), no or early (N1-N2) LN involement, no or low blood tumor burden (<1000/ul circulating sezary cells).
Stage IV
High blood tumor burden(>1000/ul) and/or extensive LN involvement (N3) or visceral involvement(M1)
LN histopathological staging
ISCL/EORTC Dutch system NCI classification
N1 1: DL, no atypical CMC LN0: no atypical lymphocytes (AL)
LN1, occasional, isolated AL
LN2: clusters (3-6 cells) of AL
N2 2. DL with early involvement LN3: aggregate of AL,
with scattered atypical CMC aeheticture preserved
N3 3. partial effacement of architecture LN4: partial or complete effacement of
W many CMC architecture w many AL
4. Complete effacement of architecture